This is an online E log book to discuss our patient's de-identified health data shared after taking his/her/guardian's signed informed consent. Here we discuss our individual patient's problems through series of inputs from global online community of experts with an aim to solve those patient's clinical problems with collective current best evidence based inputs.
This E log book also reflects my patient-centred online learning portfolio and your valuable inputs on the comment box is welcome."I've been given this case to solve in an attempt to understand the topic of "patient clinical data analysis" to develop my competency in reading and comprehending clinical data including history, clinical findings, investigations and come up with a diagnosis and treatment plan.
CHEIF COMPLAINTS :-
A 79 year old male was brought to the OPD with cheif complaints of cough since 20 days ,C/o altered sensorium since 3 days, difficulty in swallowing since 1 month and fever since 10 days
HOPI:
Patient was apparently asymptomatic 20days back then he developed cough insidious in onset and gradually progressive. PRODUCTIVE but patient is not able to spit it out. Difficulty in swallowing.
H/o cough on intake of liquids.
H/o change of voice since 20 days, insidious, hoarse in character and
SLURRING OF SPEECH +present
No h/o difficulty in breathing, breathlessness, hemoptysis
Fever since 10 days -high grade. O/e Chills and rigors + (38 spikes).
N/h/o vomiting, chest pain, loose stools.
7 YEARS BACK:(2016)
He developed head ache at around afternoon 2pm and followed by vomtings and left hand itching and weakness.
PATIENT is awake on that night due to left hand weakness and itching
NEXT DAY
MORNING they took him to hospital
Patient can lift his hand
But unable to hold objects
AFTER 3 DAYS
PATIENT became left sided hemiplegia.
MRI REPORT- 3 INFARCTS
Patient stayed for 40 days in hospital and there was no improvement and discharged.
He took liquids for 3months because patient is unable to eat solid foods.then he slowing started eating solid foods.
AFTER 1 YEAR (2017):
vomitings
Fever
Shivering for 3 days
Diagnosed with urinary tract infection
Took treatment (antibiotics) for 5 days and it resolved
AFTER 3 YEARS:(2020)
Cough for 2days
Fever on 2nd day
Diagnosed with covid
He got COVID for 1st time and resolved
After 1 year(2021)
He was Diagnosed with COVID for 2nd time and resolved
1 YEARS back (2022)
He got seizures for 5min and they took him to the hospital.
He got Typhoid fever 2times
1st time resolved in 7days
2nd time resolved in 9 days
79 Year old male who is a father of 4 children ( 2 sons and 2 daughters)..was used to run shop ( kirana shop) for about 18 years.He stopped looking after his shop from 2006 and he was looked after by his son's.
He was non alcoholic,non smoker.
10 years back , patient developed lesions on his both foot and went to the doctor and found to have diabetes and started on medication.and after 1 year ,with regular check up he was found to be Hypertensive and started on antihypertensive medication.
From 7 years onwards , patient was bedridden with foleys ( changed every 15 days ) and physiotherapy was done by his attenders daily, but there was no such improvement
PAST HISTORY
Patient is a k/c/o Hypertension and type 2 diabetes since past 10years for which he is on medications I.e tab TELMA AM 40mg po/od. Tab zoryl mv , po/od
PERSONAL HISTORY
Appetite lost,
Mixed diet
Bowel- constipated,
Bladder regular
No known allergies and Addictions.
i.e non alcoholic and non smoker
Family History- no significant family history
Treatment history
•Tab TELMA AM 40mg po/od since past 10years
•Tab zoryl mv , po/od
•Tab levipil 500mg since 2 years
• thyronorm 25mcg. Since5 years
GENERAL EXAMINATION
On examination patient is arousable but not oriented.
Pt not cooperative mostly.
-PALLOR:PRESENT
NO PEDAL EDEMA, ICTERUS, CYANOSIS, CLUBBING, LYMPHADENOPATHY
VITALS ON ADMISSION
PR-90 BPM
BP- 140/80MM HG
RR- 22 CPM
SPO2- 98% AT RA
GRBS - 183mg/dl
SYSTEMIC EXAMINATION:
Respiratory :-
Inspection : respiratory movements equal on both sides
Trachea central
palpation : apical impulse in left 5th intercostal space
Auscultation : normal vesicular breath sounds
Percussion- BAE+

CNS
PATIENT is unconscious incoherent uncooperative
HIGHER MENTAL FUNCTIONS- cannot be elecited
Speech
Behaviour
Memory
Intelligence
Lobar functions
B/L PUPILS - NORMAL SIZE AND REACTIVE TO LIGHT
NO SIGNS OF MENINGEAL IRRITATION,
CRANIAL NERVES
1. CN
Sence of Smell - N
2. CN
visual acuity - decreased on left side
3,4,6 CN
EOM movement - could not perform
Pupil size - 2, 3 mm
Direct light reflex/consensual light reflex/accommodation reflex - present, present
Ptosis - absent, absent
Nystagmus - absent, absent
5 CN
Sensory over face & buccal mucosa - N, N
Motor - masseter, Temporalis, pterigoids - N, N
Reflexes - Corneal,Conjunctival - N, N
Jaw jerk -
7 CN
Motor
Nasolabial fold - equal om both sides
Occipito frontalis - equal om both sides
Orbicularis oculi - equal om both sides
Orbicular oris - equal om both sides
Buccinator - equal om both sides
Sensory:
Taste over anterior two third of tongue - cant be performed
8 CN - could not perform
Rinnes test
Webers test
9, 10 CN -
Uvula palatal arches movements - N, N
Gag reflex - N
palatal reflex - N
11 CN - could not be elicited
Trapezius
Sternocleidomastoid
12 CN
wasting - no
Fasciculations - no
Tongue protrusion to midline - midline
SENSORY SYSTEM- cannot be elicited
Spinothalamic sensation:
Crude touch
Pain
Temperature
Dorsal column sensation
Fine touch
Vibration
Propioception
Cortical sensation
Two point discrimination
Tactile localisation
Stereognosis
Graphathesia
MOTOR EXAMINATION:
Right n left
UL. LL. UL. LL
BULK Normal Reduced
TONE Normal Hypotonia
POWER Could not be elicited
SUPERFICIAL REFLEXS
plantar reflex
Left side babinski sign positive
DEEP REFLEXES:
BICEPS, TRICEPS, SUPINATOR, KNEE ANKLE - abnormal
CEREBELLAR EXAMINATION cannot be elicited
SIGNS OF MENINGEAL IRRITATION: absent
GAIT: patient unable to walk
CVS
ASCULTATION: S1S2 +,NO MURMURS
P/A
INSPECTION: UMBILICUS IS CENTRAL AND INVERTED, ALL QUADRANTS MOVING EQUALLY WITH RESPIRATION,NO SCARS,SINUSES, ENGORGED VEINS, PULSATIONS
AUSCULTATION: no bowel sounds heard
bed sores
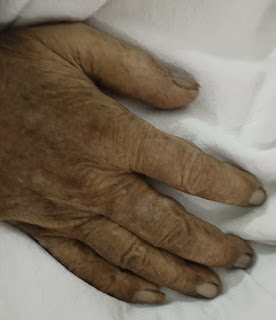
C/o asymptomatic lesions all over the body since 2 months
H/o application of unknown topical medications used
O/e multiple hyperpigmented Macclesfield present all over the body with scaly lesions over the upper back
•Diffuse xerosis present
• single ulcer of size 1.5x1.5 cms (approx) over the back.
Diagnosis SENILE XEROSIS + post inflammatory hyperpigmentation.
INVESTIGATIONS:
Anti HCV antibodies rapid -nonreactive
Blood urea -30mg/dl
HBA1C-6.7%
HbsAg rapid - negative
HIV 1/2 RAPID TEST - NON REACTIVE
TOTAL BILIRUBIN -0.81mg/dl(normal-0 to 1mg/dl)
Direct bilirubin-0.17mg/dl(0 to 0.2mg /dl)
Serum creatinine -0.9 mg/dl (0.8 to 1.3 mg /dl)
ABG
Ph 7.51
PCO2 29.5mmhg
Po2 67.5 mmhg
Electrolyte
Sodium 135meq/l
Potassium 3.5 meq/l
Chloride 98meq/l
Calcium -1.06 mmol/l
PROVISIONAL DIAGNOSIS
Recurrent CVA with hypertension, type 2 DM, seizures disorder
TREATMENT
1) TAB ECOSPRIN 150 mg RT/OD
2) TAB CLOPIDOGREL 75 MG RT/OD
3) TAB ATORVAS 20 MG RT/OD
4) NEBULISATION - 3% NS ,
MUCUMZY 8th hourly
5) CHEST PHYSIOTHERAPY.
6) RT FEEDS 100 ML WATER 2nd HRLY
50 ML Milk 2nd HRLY.
7) TAB. THYRONORM 25MCG RT/OD
8) TAB. LEVIPIL










Comments
Post a Comment